Author: abigail_admin
Placental Variations During Pregnancy
By Dr Abby Evans
During pregnancy, the placenta is one of the most remarkable organs your body creates. It develops specifically to support your baby, delivering oxygen, nutrients and hormones while removing waste products.
Most of the time, the placenta forms in a fairly standard way. It attaches to the wall of the uterus, grows into a round disc shape, and the umbilical cord inserts somewhere near the centre. But like many things in pregnancy, there can be variations in how the placenta forms.
These differences are often picked up on ultrasound or noticed after birth when the placenta is examined.
Hearing unfamiliar terms related to the placenta can sometimes cause unnecessary anxiety, so it helps to understand what these variations actually mean.
Why placental structure can vary
The placenta develops from early pregnancy tissue and grows rapidly during the first trimester. As it expands across the uterine wall, small differences in how the tissue forms or where blood vessels travel can lead to variations in its appearance. Importantly, many of these variations are simply anatomical differences rather than medical problems.
Variations in placental lobes
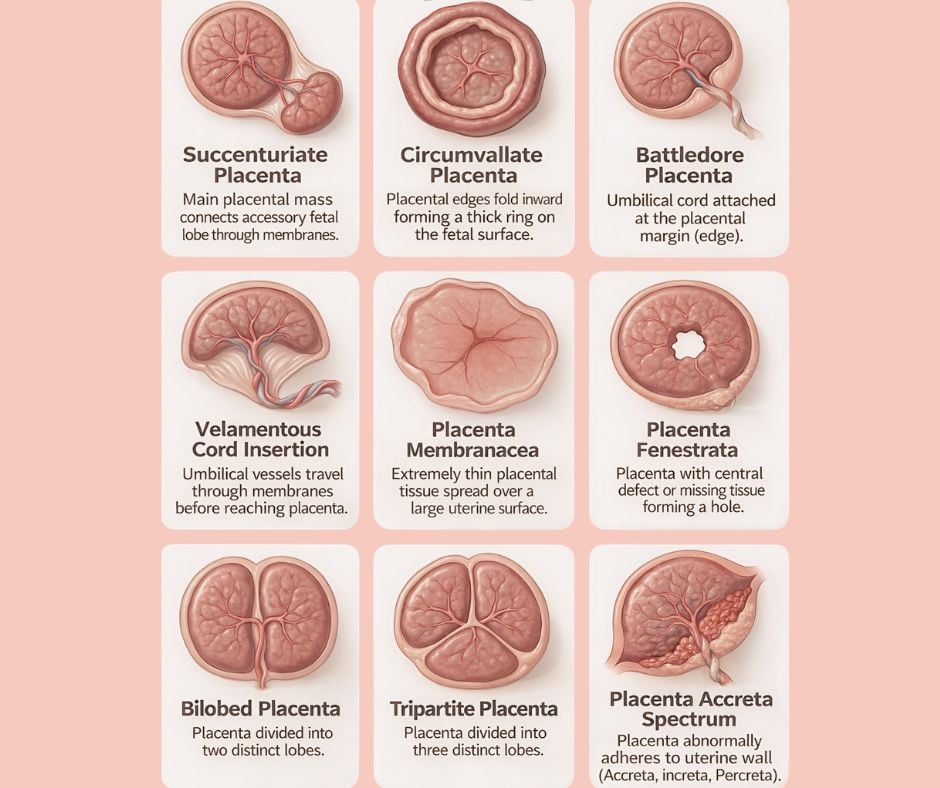
Sometimes the placenta forms with more than one section, or “lobe”. A bilobed placenta means the placenta has two main sections connected by blood vessels. A tripartite placenta has three lobes instead of one. There is also a variation called a succenturiate lobe, where a small accessory lobe develops separate from the main placenta but remains connected through the membranes. Most of the time these findings do not cause complications, but knowing they are present helps guide monitoring during pregnancy and ensures that the entire placenta is delivered safely after birth.
Differences in cord attachment
Another variation relates to where the umbilical cord attaches. Normally the cord inserts near the centre of the placenta, but sometimes it attaches closer to the edge. This is called a battledore placenta. In a rarer variation known as velamentous cord insertion, the cord vessels travel through the membranes before reaching the placenta rather than being protected within the placental tissue itself. When identified on ultrasound, this can simply mean we monitor the pregnancy a little more closely to ensure blood flow to the baby remains optimal.
Variations in placental shape
Occasionally the placenta develops structural differences in its surface. A circumvallate placenta occurs when the edges of the placenta fold inward, forming a raised ring around the outer edge. Another rare variation is placenta membranacea, where placental tissue spreads thinly across a wider area of the uterus. There are also uncommon findings such as placenta fenestrata, where a small central gap appears within the placental tissue. Many of these are simply interesting anatomical findings rather than something that affects pregnancy significantly.
Placenta accreta spectrum
One placental condition that does require careful planning is placenta accreta spectrum. This occurs when the placenta attaches too deeply into the wall of the uterus. Depending on the depth of attachment, this can be classified as accreta, increta or percreta. Fortunately this is relatively uncommon, but when identified during pregnancy it allows the obstetric team to carefully plan delivery to ensure the safest outcome for both mother and baby.
Why monitoring matters
One of the reasons routine ultrasound scans are so valuable is that they allow us to identify placental position and structure during pregnancy. Most placental variations do not affect the course of pregnancy, but knowing about them helps us tailor care when necessary.
Every pregnancy is unique
The placenta is a temporary but incredibly complex organ, and no two pregnancies are exactly the same. Variations in placental shape, lobes or cord insertion are often simply part of the natural diversity of pregnancy. What matters most is careful monitoring, good communication and a care plan that supports both mother and baby throughout the pregnancy journey.
Dr Abby
When Something Feels “Off” – Understanding Vulval and Vaginal Conditions

Many women experience changes, discomfort, or irritation in their vulva or vagina at some point in their lives, but too often, they feel
awkward bringing it up. Whether it’s itching, burning, pain, or changes in skin texture, these symptoms are worth attention, not embarrassment.
I thought I would talk about some of the more common vulval and vaginal conditions, how
they present, and when to seek help. And I hope this helps whoever is reading this.
Vulval irritation and itching
Irritation can happen for many reasons, and not all of them are infections.
● Dermatitis or allergic reactions: Fragranced soaps, pads, or laundry detergents are
common culprits.
● Lichen sclerosus: A chronic skin condition that causes thin, white, itchy patches on
the vulva. It’s not contagious, but it does need long-term management to prevent
scarring or narrowing of the vaginal opening.
● Lichen planus: Similar to lichen sclerosus but can affect the vagina as well,
sometimes causing soreness or small erosions.
These conditions often need topical prescription creams and ongoing monitoring, not
over-the-counter antifungal treatments, a reason why you need to seek proper medical
advice.
Pain and burning
Pain or burning in the vulva or vagina isn’t “normal,” even if you’ve been told it’s just
sensitivity. Possible causes include:
● Vulvodynia: Chronic pain without an obvious cause. It can feel like burning, stinging,
or rawness, often triggered by touch, sex, or even tight clothing.
● Atrophic vaginitis: Thinning of the vaginal tissue due to low oestrogen, especially
after menopause, breastfeeding, or long-term hormonal suppression.
● Infections: While yeast infections and bacterial vaginosis are common, if treatment
isn’t working, further testing may be needed to confirm the cause.
Persistent pain deserves a proper assessment, including a gentle physical exam and
sometimes swabs or a biopsy to clarify the diagnosis.
Changes in skin, discharge, or appearance
Noticing a lump, bump, colour change, or patch of thickened skin on the vulva can be
unsettling. Most are benign (like cysts or skin tags), but occasionally, they can indicate a
precancerous or cancerous change.
Warning signs to have checked include:
● Persistent pain or itching that doesn’t settle
● Ulcers or raised patches
● Bleeding, cracking, or pigment changes in the vulval skin
● Unusual or persistent discharge
Early assessment makes a huge difference. Vulval and vaginal cancers are rare, but
catching them early leads to far better outcomes.
Why women delay seeking care
Many women hesitate to bring up these types of symptoms. Sometimes it’s embarrassment;
sometimes it’s the assumption that discomfort is “just normal” after childbirth, menopause, or
ageing. Others have been dismissed in the past or told it’s “in their head.”
But your comfort, confidence, and sexual wellbeing matter.
At SHE Medical, we aim to make these conversations straightforward, respectful, and
private. You deserve to feel comfortable in your own body and to get answers when
something doesn’t feel right.
If you’ve noticed ongoing vulval or vaginal changes, irritation, pain, itching, or anything new –
please don’t ignore it. Most conditions are manageable with the right treatment plan, and
early assessment helps rule out more serious causes.
Your body is speaking to you. We’re here to listen.
Dr Sean Holland
Itching, burning, or unusual changes in the skin of your vulva or vagina?

Itching, burning, or unusual changes in the skin of your vulva or vagina can be a symptom of vulvar or vaginal dermatoses. This common and yet uncomfortable skin condition affects many women.
Symptoms can include:
- Persistent itching or burning
- Rashes, redness, or white patches
- Pain during intercourse or urination
These signs can point to conditions like lichen sclerosus, eczema, or psoriasis. If over-the-counter treatments aren’t helping, it’s important to see a gynaecologist who specialises in these issues. We can diagnose and treat the condition properly, preventing complications and improving your comfort.
Please don’t wait, early treatment is key to managing symptoms and maintaining your vulvar health. Reach out if you’re experiencing persistent symptoms. These symptoms are not pleasant so you want to get onto it as soon a possible.
Can genetic testing improve your chances of a successful IVF pregnancy?

When embarking on your fertility journey, understanding all of your options can make a world of difference. Preimplantation Genetic Screening (PGS) and Preimplantation Genetic Diagnosis (PGD) are advanced techniques that can screen embryos for genetic conditions before they are implanted, helping reduce the risk of inherited disorders and improving the likelihood of a healthy pregnancy.
This testing is done by expert embryologists at QFG, and we will provide guidance, care, and the reassurance that you’re in good hands every step of the way.
At SHE medical we understand that every family’s journey is unique, and we’re here to help you navigate the complexities with compassion and expert advice. If you’re exploring IVF or considering genetic testing as part of your treatment plan, let’s talk about how we can help you create the future you’ve been dreaming of.